Bariatric surgery
Surgical treatment for weight reduction can be carried out if a person’s BMI is over 35 and if weight reduction through dieting has been tried for a cumulative period of 2 years. If a person’s BMI is more than 50, surgery can be considered if dieting has been tried for one year without significant or lasting weight loss.
Bariatric surgery is very complex and one of the most specialized abdominal surgeries.
The GDK (www.gdk-cds.ch, can be found under highly specialized digestive surgery: complex bariatric surgeries) has granted the mandate to execute complex bariatric interventions only to a few hospitals in Switzerland.
The quality of surgical obesity treatment depends on the following factors:
- Does the hospital have a specialized interdisciplinary team that examines and clarifies individual cases before surgery, and supervises after the operation?
- Does the hospital run a 24-hour emergency operation service on 365 days of the year, and is staffed with chief physicians?
- Does the hospital have a recognized ICU with ventilator places?
- 4 Will an experienced surgical team operate you?
The previous experience and number of operations performed by the surgeon is an important factor contributing to a low complication rate.
An experienced bariatric surgeon has performed at least 500 surgeries himself, and he knows several surgical techniques impeccably. In addition he should carry out at least 50 bariatric procedures per year.
Please always inquire about these points as a patient or relative!
Results and goals

: Emanuel Freudiger
We pursue the following objectives with bariatric surgery:
- Long-term and sustainable weight reduction of at least 50% of excess weight.
- Improvement in our patients’ quality of life.
- Reintegration of our patients into «working life» and improved social contacts.
- Curing, or at least improving, the secondary diseases of obesity (e.g. diabetes, hypertension, etc.)
Bariatric surgery is not a «lifestyle» surgery. It is not about operating on people to create slenderness. Bariatric surgery treats the disease obesity and the secondary diseases linked to obesity, and offers obese people the opportunity to guide their lives in a healthier direction.
An interdisciplinary team (consisting of internists, nutritionists and surgeons) will inform you further and advise you on the various surgical techniques. After a joint assessment of your case within the interdisciplinary team, we will decide whether you qualify for a surgical procedure for weight loss.
The time between the first consultation and surgery is usually 3 to 4 months. After the operation, the patient needs lifelong follow-ups, which are done by the interdisciplinary team.
If you encounter chronic abdominal pain after bariatric surgery, or if you lose insufficient weight after the operation, you should consult an experienced interdisciplinary team in order to obtain further support.
Below you can find the various bariatric surgeries we offer.
Please visit the website of the Limmattal hospital (www.spital-limmattal.ch) for further information about our interdisciplinary team.
Gastric band
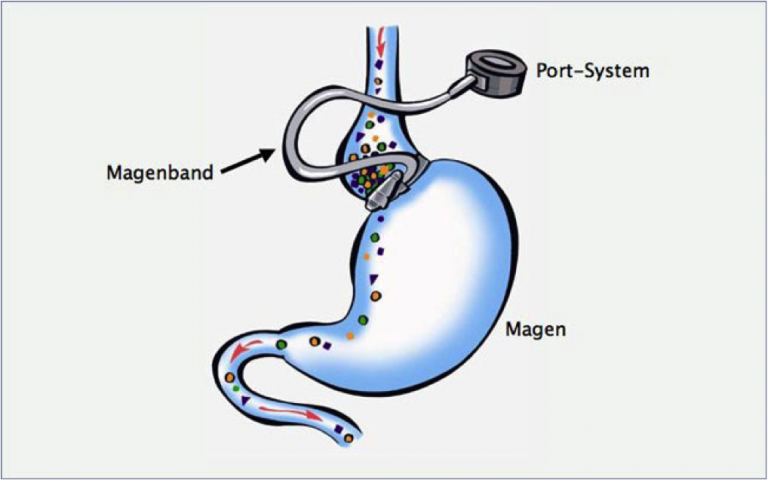
The gastric band is made out of silicone and is placed like a ring around the upper part of the stomach. The stomach band is connected via a tube system with a «reservoir» system that is implanted under the skin. This «reservoir» system can be penetrated with a needle from the outside. By doing so, the gastric band can be adjusted tighter or looser (see sketch).
You can lose an average of 50 % of your excess weight in the long term with a gastric band. However, the quality of life after gastric banding is reportedly lower than after a gastric bypass or a gastric sleeve operation. Weight loss occurs after gastric banding due to the constriction of the stomach by the band, which allows for less food intake.
After gastric binding surgery you are usually hospitalized for 1 – 3 days. The first «adjustment» of the gastric band is done after 6 weeks in conjunction with x-ray checks. Further adjustments are done based on the individual needs of the patient.
The gastric band surgery is a very safe operation with an extremely low complication rate in the first days and months. Some common late complications that have been reported, years after the operation, are the sac-like enlargement of the esophagus (secondary esophagus compensation) and the slippage of the gastric band. Due to these late complications 40 to 50 % of gastric bands have to be removed again.
The gastric band can also be used in addition to the gastric bypass, provided that this is considered a possible and useful treatment after inadequate weight loss following a gastric bypass.
Please visit the bariatric department of the hospital Limmattal during consultation hours for further information on risks and benefits of a gastric band surgery.
Gastric bypass
(Proximal gastric bypass, distal VVLL gastric bypass, Omega-gastric bypass)
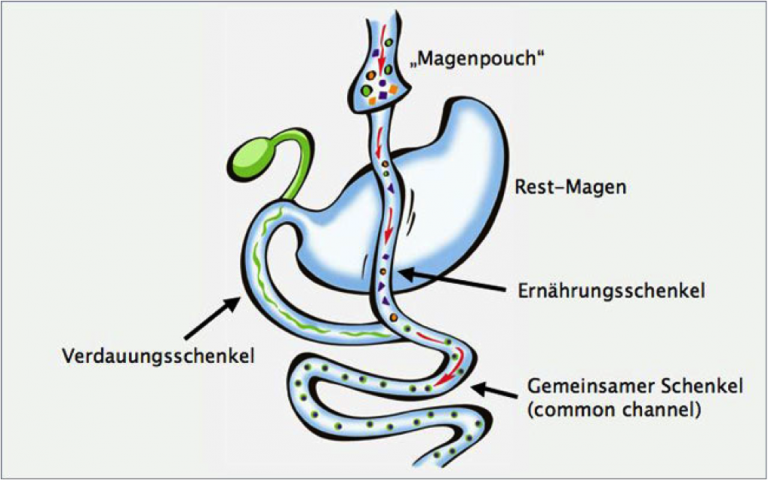
For a gastric bypass, the stomach is cut very high up and connected with a loop of the small intestines that had previously also been cut. Therefore only small meals can be eaten and satiety is reached earlier. The section of the small intestine which carries the digestive juice is reconnected with the food carrying section of the small intestine 2.5 meters (proximal gastric bypass) or 1 meter (distal gastric bypass) before the small intestine connects into the large intestine.
For an Omega gastric bypass only one connection between the stomach pouch and small intestine is established. This results in 2 meters of the small intestine no longer being used as part of the digestion process. The majority of the small intestine is being bypassed reducing the absorption of the energy carriers (fat, sugar, proteins) and, therefore, leading to weight loss.
The gastric bypass has excellent long-term results. Most patients report a good quality of life after a gastric bypass operation.
After a gastric bypass an average of 65 to 70 % of your excess weight can be lost in the long term. In addition, most secondary diseases linked with obesity can be cured or greatly improved (see comorbidities and secondary diseases of obesity).
After a gastric bypass operation you are usually hospitalized for 3 – 7 days. The very rare complications of a gastric bypass (< 0.5 %) in the early phase after the operation (first week) may include secondary bleeding or an anastomotic leak (opening of the mechanical staple seam between the intestines and stomach). The very rare late complications after a stomach bypass include malnutrition and vitamin deficiency symptoms. These possible late complications can be mostly avoided though if you comply with the necessary medical checks, together with blood tests in order to analyse your nutrition status.
Any gap created between the small intestine loops after the gastric bypass is closed by myself immediately so that the risk of internal hernias with intestinal obstruction is below 0.7 %, even years after the gastric bypass operation.
Please visit the bariatric department of the hospital Limmattal during consultation hours for further information on risks and benefits of a gastric bypass operation.
An informative android app can be found at: www.mein-magenbypass.ch
Gastric sleeve

During a sleeve gastrectomy, a thin stomach tube is formed and a large portion of the stomach is removed. In comparison with gastric bypass surgery this procedure has equally good results in weight loss after 5 years. Post operative quality of life is reportedly good. Nowadays gastric sleeve surgery is an established operative method for weight loss.
This operation has been carried out for a shorter period of time in a standardized way than the stomach bypass. As a result no definitive statements can be made for its long-term benefits. The effectiveness of the gastric sleeve (see sketch) is based on the fact that you have to eat smaller portions and the state of satiation is reached earlier. In addition, the gastric sleeve (like the stomach bypass) causes a decrease of appetite hormones, which has a favorable effect on weight reduction.
After a sleeve gastrectomy you are usually hospitalized for 3 – 7 days. The very rare complications after sleeve gastrectomy surgery (approx. 1-2%) may include secondary bleeding in the first 24 hours and the opening of the mechanical staple seam in the stomach during the first 10 days.
Severe malnutrition after a gastric sleeve operation is a rarity (< 0.1 %). Vitamin deficiencies can be avoided if you adhere to the prescribed follow-up medical visits. If the gastric tube does not lead to satisfactory weight loss after several years, it can be converted into a gastric bypass or into a «duodenal switch».
Please visit the bariatric department of the hospital Limmattal during consultation hours for further information on risks and benefits of a sleeve gastrectomy surgery.
Biliopancreatic diversion
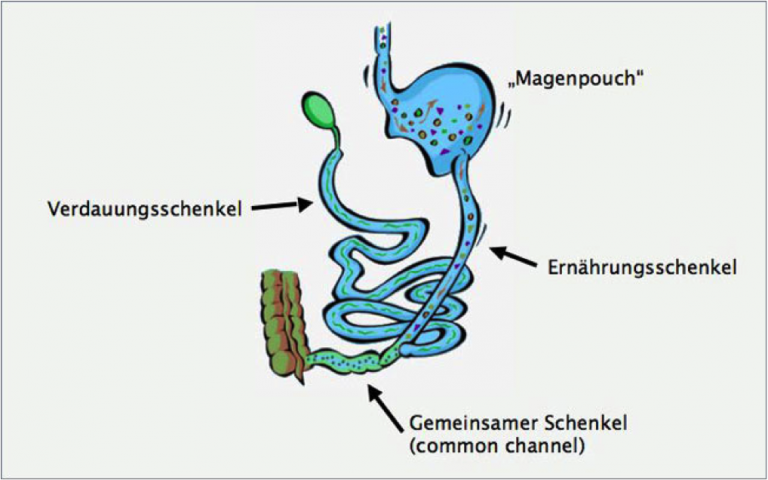
The biliopancreatic diversion can be compared structurally with gastric bypass surgery. In contrast to a gastric bypass however, a much larger part of the small intestine is circumvented from the nutrition system. The resulting weight loss is mainly due to changing the length of the small intestine and therefore less energy carriers (fats, sugars, proteins) have the opportunity to be absorbed from the food into the body.
Biliopancreatic diversion has excellent long-term weight loss results. Most patients report a good quality of life after a biliopancreatic diversion. On average, 75 to 85 % of excess weight can be sustainably lost in the long term with this procedure. In addition, most secondary diseases linked with obesity can be greatly improved or cured.
One disadvantage of the biliopancreatic diversion is the common occurrence of nutrition deficiencies and, therefore, we cannot recommend this operation routinely. However, the surgery is suitable for very severely obese patients (BMI >50) as the first, or second, alternative measure after a gastric bypass or a gastric sleeve, and is possible if the desired results could not be achieved with these initial strategies. Assessment for such an intervention must be made very carefully.
After a biliopancreatic diversion you are usually hospitalized for 5 – 7 days. The very rare complications of a biliopancreatic diversion (<1%) in the early phase after the operation may include secondary bleeding or an anastomotic leak (opening of the mechanical staple seam between intestines and stomach).
The later complications after a biliopancreatic diversion include malnutrition, vitamin deficiency symptoms, anemia, osteoporosis, and gall or kidney stones. In addition, malodorous stools and passing gas may occur often. These possible later complications can be mostly avoided if the patient complies with the necessary medical checks, together with blood tests, in order to analyse nutritional status.
Please visit the bariatric department of the hospital Limmattal during consultation hours for further information on risks and benefits of a biliopancreatic diversion.
FAQ
Does health insurance cover bariatric surgery?
The requirements for health insurance companies to cover such surgery include:
- BMI > 35
- Extended efforts to diet for a minimum of two years, or in some cases, one year.
Moreover, you should not suffer from any other serious psychiatric or medical condition.
How much weight can I lose after bariatric surgery?
Each bariatric surgery method can lead to sustainable and long-term weight loss. However, with each method of surgery there is also the possibility that the desired results cannot be achieved.
Numerous studies, which are consistent with our numbers and experience, provide a statistical average of weight loss for each individual intervention. In the first 5 years you can expect to lose approximately 65 – 70 % of excess weight with a gastric bypass, 50 – 55 % with a gastric band and 50 – 65 % with a stomach tube.
The weight loss usually occurs within a year. After that your weight will settle down to a new level. Cases of being «underweight» after bariatric surgery are rare.
Is bariatric surgery dangerous? Are there many complications? Or is it more dangerous if I stay overweight (BMI > 35)?
Bariatric surgery completed by an experienced surgery team is not considered dangerous. Nevertheless, as with any surgery, complications can occur and are, in some cases, severe. In very rare cases these complications can be fatal.
The «death rate» after bariatric surgeries is below 0.5%.
This death rate after surgery has to be compared with the death rate due to excess weight. If compared in the long-term, the death rate for bariatric surgery patients is much lower than that for obese patients with a BMI > 35 who have not had surgery. Numerous long-term studies show that obesity is much more dangerous for your health than a surgical intervention due to the many secondary diseases that can develop.
Shall a robot do the operation?
The so-called robotic surgery has not prevailed in bariatric surgery, as it is not advantageous for the patient. The abdominal incisions are the same size as with a conventional laparoscopy. A skilled surgeon is much faster with the conventional laparoscopy than with robotic surgery. Robotic surgery unnecessarily prolongs the anesthetic time in bariatric surgery and does not lower the complication rate.
Essentially, with robotic surgery the operation is still done by the surgeon, however, the surgeon does not stand at the operating table but sits at a console and moves the instruments via a joystick.
There are clinics that charge a premium of several thousand francs for robotic bariatric surgeries without a real benefit for you as the patient.
I received a gastric bypass weeks or months ago and since then I cannot eat well.
If you vomit immediately after food intake and if this problem started only a few weeks after the operation, then it is possible that the connection between the stomach and small intestine (gastroenterostomy) has scarred too thickly.
Please contact the bariatric department of the hospital Limmattal during consultation hours so we can clarify the cause. A narrowing of the gastroenterostomy can be successfully dilated with a balloon through a gastroscopy.
After food intake I feel very tired, sometimes I feel sick. I sweat and sometimes everything goes black.
If you are suffering from these or similar symptoms, «dumping syndrome» might be the reason. Dumping syndrome is often seen after gastric bypass, duodenal switch or biliopancreatic diversion surgery.
It is a disorder of your glucose metabolism. Often this disorder is caused by a too rapid or excessive consumption of carbohydrate rich foods. Carbohydrates are in all sweet dishes and drinks (chocolate, tiramisu, ice-tea, Coca-Cola, etc) but also in bread and pasta. If you think that you are suffering from dumping syndrome contact the bariatric department of the hospital Limmattal during consultation hours immediately.
After the gastric bypass surgery my stools are more liquid and very smelly. What can I do about this?
The stool changes in most cases after distal VVLL gastric bypass surgery. The changes, however, are very individual. The malodorous stools occur especially when undigested fat is excreted in the stool. You can avoid this if you limit your intake of fatty foods (fondue, raclette, cordon-bleu, crisps, hamburgers, etc.).
If you suffer from chronic diarrhea visit the bariatric department of the hospital Limmattal during consultation hours.
I am experiencing repeated abdominal pain after the bariatric surgery. What can I do?
Slight abdominal pain after bariatric surgery is common and the reasons are varied and mostly harmless. Often the pain is caused by a dietetic mistake.
If you suffer of abdominal colic (especially in the right upper abdomen) gallstones could be the reason for the pain. If you suffer from sudden, strong and diffuse abdominal pain, we recommend an immediate inpatient clarification of the reason via the emergency ward of the hospital Limmattal. The reason may be twists of the intestines or internal hernias.
Can I get pregnant after bariatric surgery? Is there an increased risk for the pregnancy after bariatric surgery?
After bariatric surgery you can become pregnant without any problems. However, we recommend waiting 12 months after the surgery. It is important to have your blood vitamin and nutrition levels checked on a regular basis, especially when pregnant. Studies show that the associated risks to pregnant women is higher when they are obese (BMI >40) than after a gastric bypass surgery. Therefore, we recommend carrying out a planned bariatric surgery before a planned pregnancy.
I am developing an excess of skin after losing weight. What can I do?
There is no way of predicting if you will suffer from excess skin after successful weight reduction. Unfortunately, there are no reliable preventative measures to avoid the excess skin formation. Typical areas for excess skin are the abdomen, hips, thighs, breasts and arms.
The excess skin formation can only be treated surgically. Please talk to the bariatric department of the hospital Limmattal during consultation hours if you suffer from excess skin formation so that we can take further steps.
What if I regain weight after the surgery?
A slight weight gain 2 to 4 years after the bariatric surgery is normal.
However, a bigger weight gain must be investigated. There are many possible reasons for renewed weight gain. Our interdisciplinary team will begin the necessary inquiries and will advise you about the various therapy options.